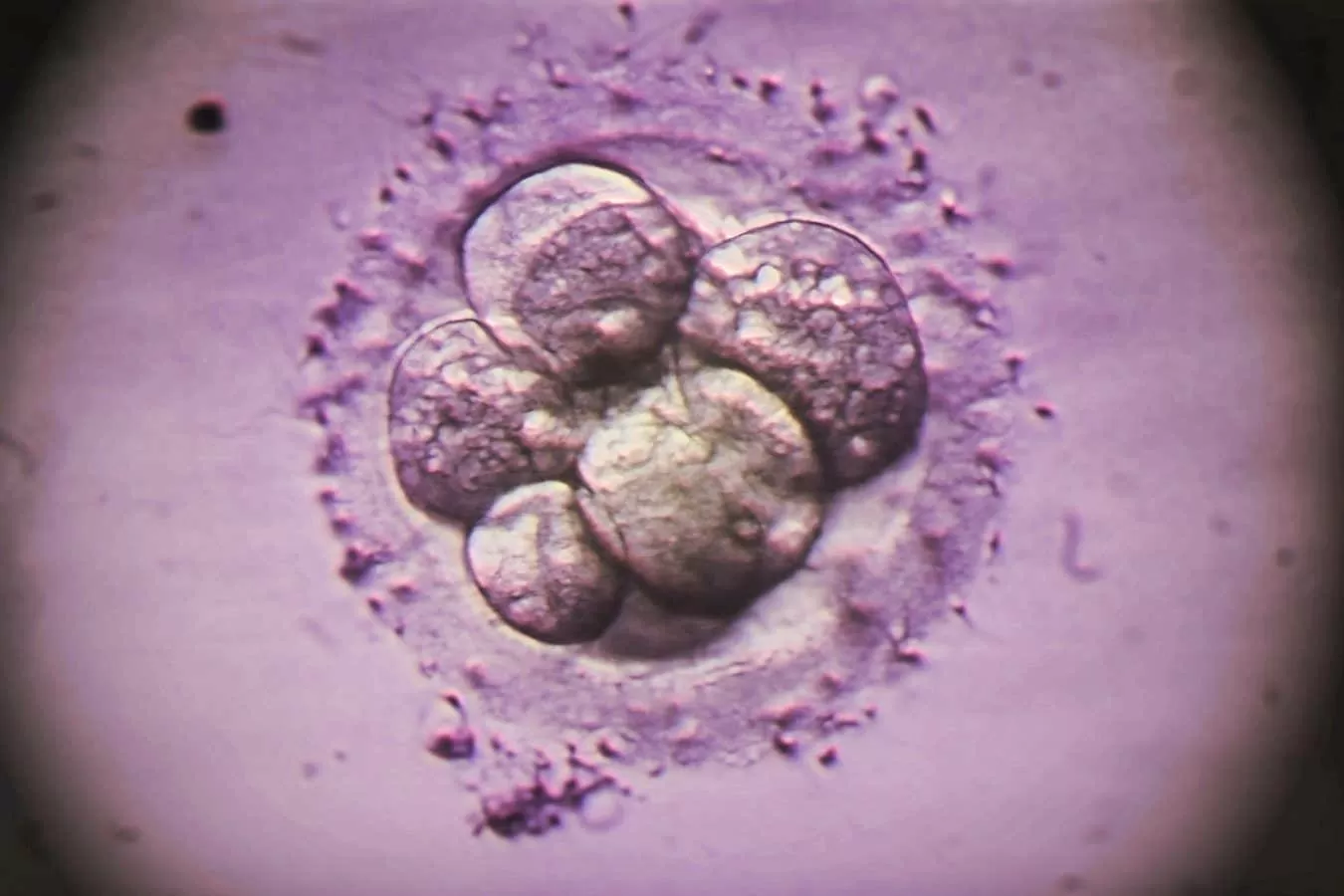
In vitro fertilisation (IVF) has been a groundbreaking technology in the field of reproductive medicine, giving hope to millions of couples struggling with infertility. This assisted reproductive technique involves the fertilisation of an egg with sperm outside the body, followed by the transfer of the resulting embryo into the uterus. While IVF has helped many couples achieve their dream of having a child, it is not without its challenges and controversies.
One of the concerns surrounding IVF is the potential for genetic abnormalities in the embryos formed through this process. This is a valid concern, as genetic testing is often performed on embryos before they are implanted into the uterus. This testing is done to identify any potential genetic disorders or chromosomal abnormalities that may affect the health of the baby. However, recent studies have shown that embryos formed with IVF can develop genetic abnormalities in the time between testing and implantation.
This may sound alarming, but it is important to understand that this does not necessarily mean that the embryos are not viable. In fact, many of these abnormalities are minor and do not have a significant impact on the health of the baby. It is also important to note that these abnormalities can occur in natural conception as well, but they are not usually detected until after the baby is born.
So, how does this happen? During IVF, eggs are retrieved from the woman’s ovaries and fertilised with sperm in a laboratory. The resulting embryos are then grown in a controlled environment for a few days before being tested for genetic abnormalities. However, during this time, the embryos are still developing and can undergo changes that may result in genetic abnormalities. This is known as mosaicism, where some cells in the embryo have a different genetic makeup than others.
Mosaicism is not uncommon and can occur in up to 20% of embryos formed with IVF. It is important to note that not all mosaicism leads to genetic abnormalities, and many embryos with this condition can still result in a healthy baby. In fact, a recent study published in the New England Journal of Medicine found that only 1.4% of embryos with mosaicism resulted in a child with a genetic disorder.
Furthermore, the technology used for genetic testing of embryos is constantly improving, making it more accurate and reliable. This means that the chances of detecting any potential abnormalities are higher, and the risk of transferring an embryo with a genetic disorder is significantly reduced.
It is also worth mentioning that the majority of IVF clinics have strict protocols in place to ensure the safety and well-being of their patients. This includes regular quality control checks and following guidelines set by regulatory bodies. These measures help to minimise the risk of genetic abnormalities in embryos formed through IVF.
So, what does this mean for couples undergoing IVF? It is important to understand that while there is a small risk of genetic abnormalities in embryos formed through IVF, the chances of having a healthy baby are still high. It is also crucial to have open and honest communication with your doctor about any concerns or questions you may have. They can provide you with the necessary information and support to make informed decisions about your treatment.
In conclusion, while it is true that embryos formed with IVF can develop genetic abnormalities in the time between testing and implantation, this does not necessarily mean that they are not viable. The technology used for genetic testing is constantly improving, and the chances of detecting any potential abnormalities are higher than ever. IVF remains a safe and effective option for couples struggling with infertility, and the joy of having a child far outweighs any potential risks. Let us continue to support and celebrate the advancements in reproductive medicine, giving hope to those who dream of starting a family.